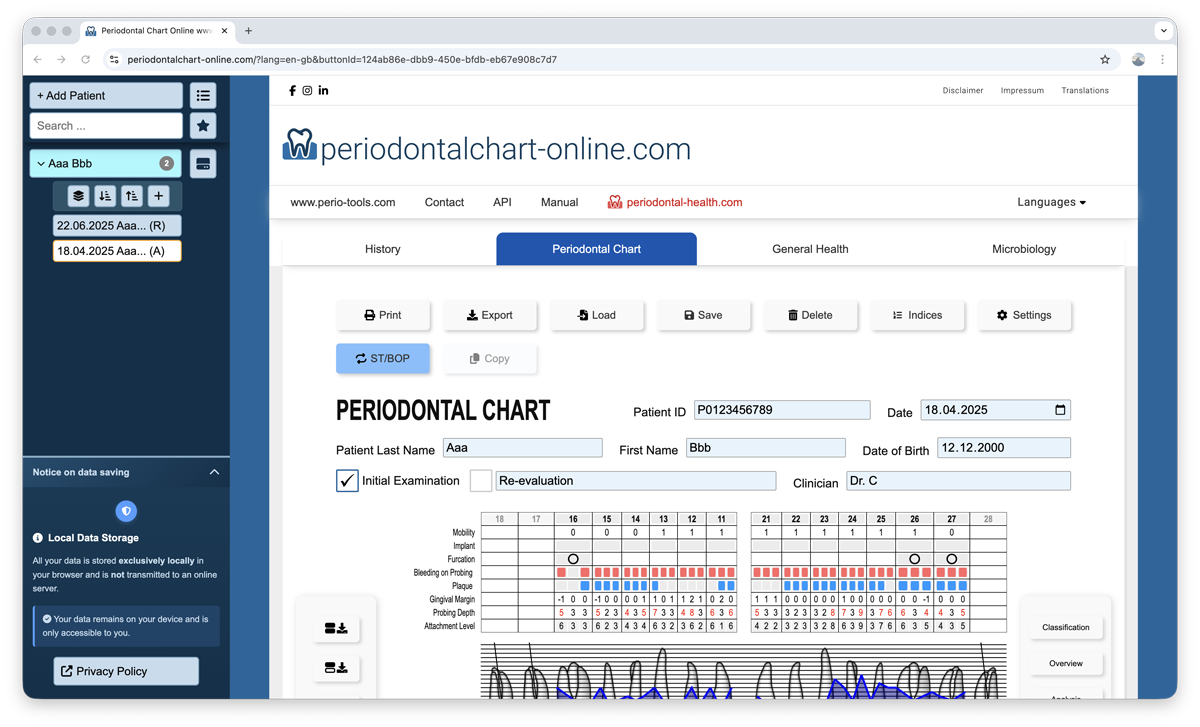
2. Periodontal Chart Tab
The Periodontal Chart tab is used to record and visualize the clinical periodontal examination. It allows for the input of patient information, clinical measurements, and the visualization of findings.
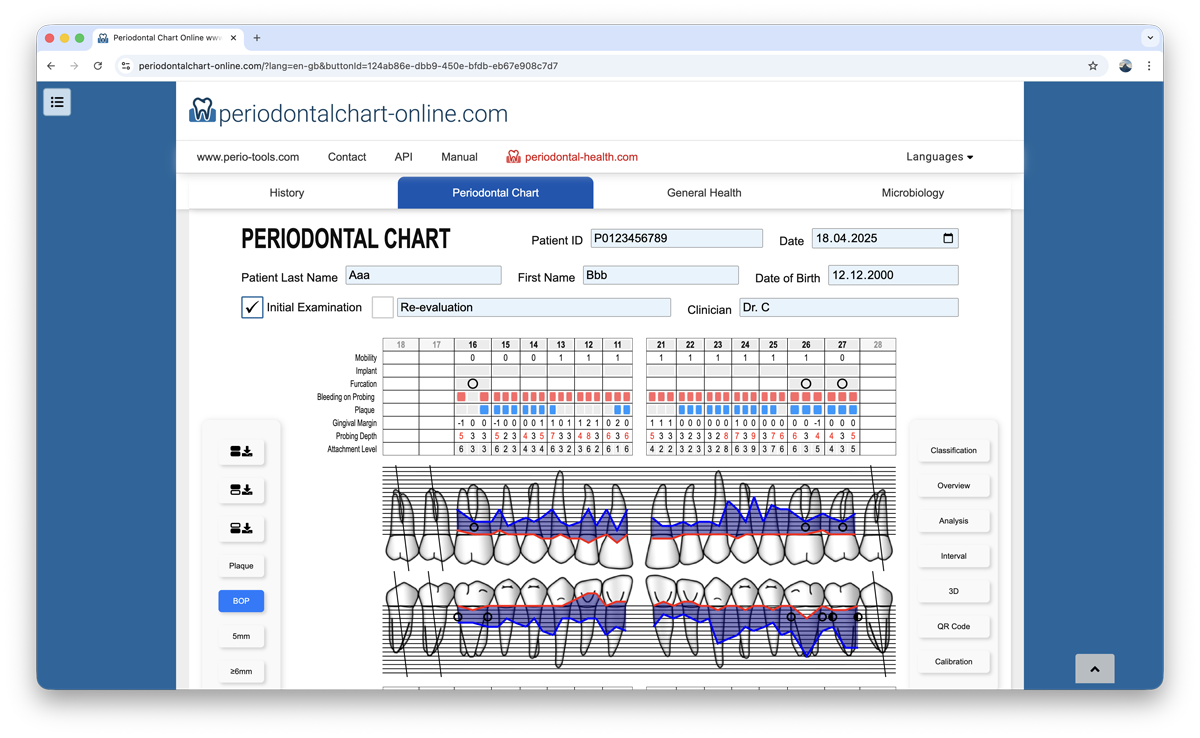
Patient and Examination Information
At the top, entry fields are available for patient information, clinician name, and examination type (Initial or Re-evaluation).
Recording Teeth and Implants
- Missing Teeth: Click on the tooth number to cross it out.
- Implant Status: Use the implant button to cycle through states:
- First click: implant present
- Second click: implant marked in red (e.g., peri-implantitis)
- Third click: implant marked in green (e.g., successfully treated peri-implantitis)
- Fourth click: implant is removed and position returns to natural tooth
Clinical Parameters and Indices
Measurements are typically recorded at six sites per tooth. The application supports various clinical indices categorized as follows:
1. Probing Depth, Gingival Margin and Attachment Level
- PD (Probing Depth): Measured in millimeters at 6 sites per tooth.
- GM (Gingival Margin): Measured in millimeters relative to the cemento-enamel junction (CEJ).
- AL (Attachment Level): Automatically calculated as the sum of PD and GM (AL = PD + GM).
2. Oral Hygiene Indices
- Plaque (O'Leary et al. 1972): Recorded as binary (0/1) to calculate the full-mouth plaque score. [Standard]
- PI (Silness and Löe 1964): Plaque Index for assessing the thickness of plaque at the gingival margin.
- mPI (Mombelli et al. 1987): Modified Plaque Index specifically designed for dental implants.
3. Gingivitis and Peri-Implant Mucositis
- BOP (Bleeding on Probing): Bleeding according to Lang et al. (1986), recorded as 0 (no bleeding) or 1 (bleeding). [Standard]
- GI (Gingival Index): Assessment of gingival inflammation according to Löe and Silness (1963).
- mGI (Modified Gingival Index): Inflammation assessment for implants according to Mombelli et al. (1987).
4. Recessions and Advanced Parameters
For clinical practice and clinical studies, additional indices are available to record parameters at either 2 or 6 sites per tooth:
- REC Mi: Recession classification according to Miller (1985).
- REC Ca: Recession classification according to Cairo et al. (2011).
- REC X / REC Y: Custom recession values (2 or 6 values per tooth).
- KG (MGJ): Width of Keratinised Gingiva (Mucogingival Junction) in mm.
- GT (Gingival Thickness): Evaluation of the gingival phenotype (thin/thick).
- W (Width): Measured width in mm according to Pandey & Mehta (2013).
- CEJ: Documentation of the visibility of the Cemento-Enamel Junction.
- Step: Evaluation of root surface concavities.
- Tooth Mobility: Recorded following the Miller (1950) mobility classification.
- Clicking the labels "Bleeding on Probing" or "Plaque Index" will fill the entire row with positive values (BOP+ or PI+).
- Using Shift+Click on these labels will clear all entries in that row.
- Alternatively, you can hold down the Shift key while moving the mouse over the BOP or Plaque areas to toggle these sites.
Copy Values from Last Examination
When creating a new charting record for a patient who already has existing examinations, the system offers a "Copy Values" dropdown menu. This feature is particularly useful for transferring baseline data that may not have changed since the last visit:
- Parameters: You can selectively copy Tooth Status (including implants), Furcation grades, Probing Depths (PD), Gingival Margin (GM), Bleeding on Probing (BOP), and Plaque Index (PI).
- Availability: This copy function is available for a time window of 5 minutes after the new chart is created.
- Reversibility: The transfer is interactive: clicking the same field in the dropdown again will immediately undo the data transfer.
Automatic Calculations
In the center of the periodontal chart, summary values are calculated automatically:
- Mean probing depth (one decimal place)
- Mean attachment level (one decimal place)
- Bleeding on Probing percentage (BOP%)
- Plaque Index percentage (PI%)
Comparative Overlay
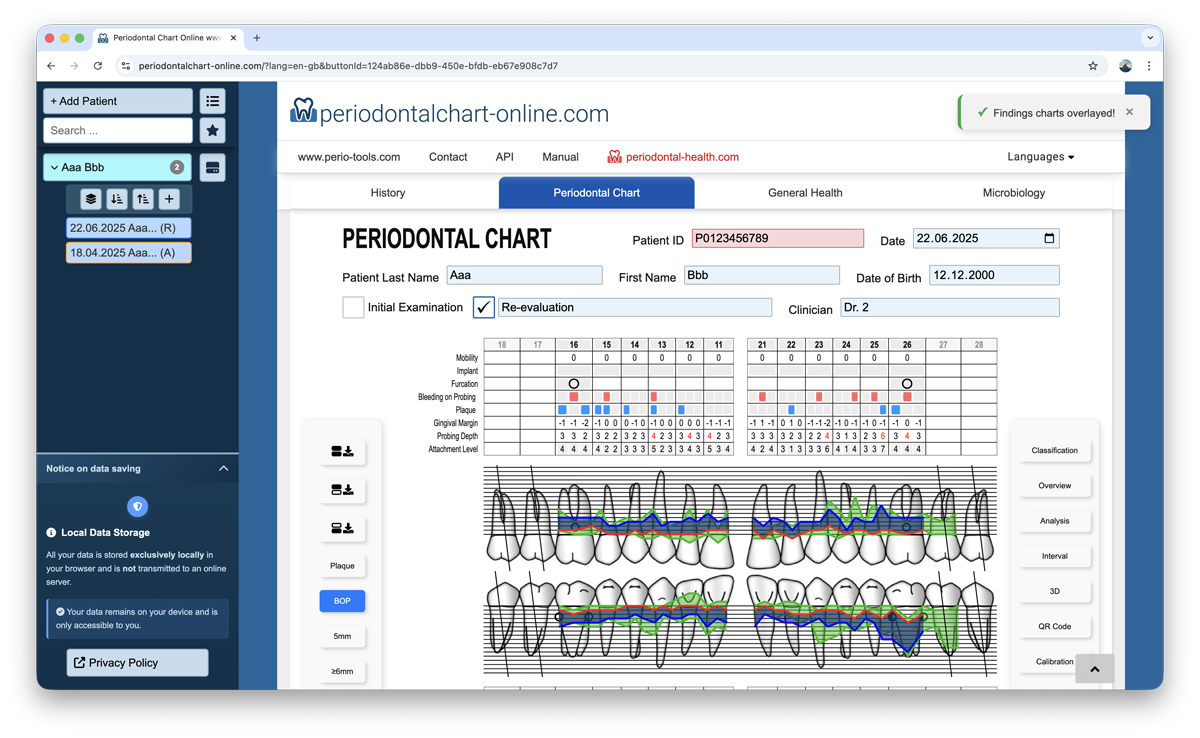
Settings
The Settings menu allows customization of the periodontal chart:
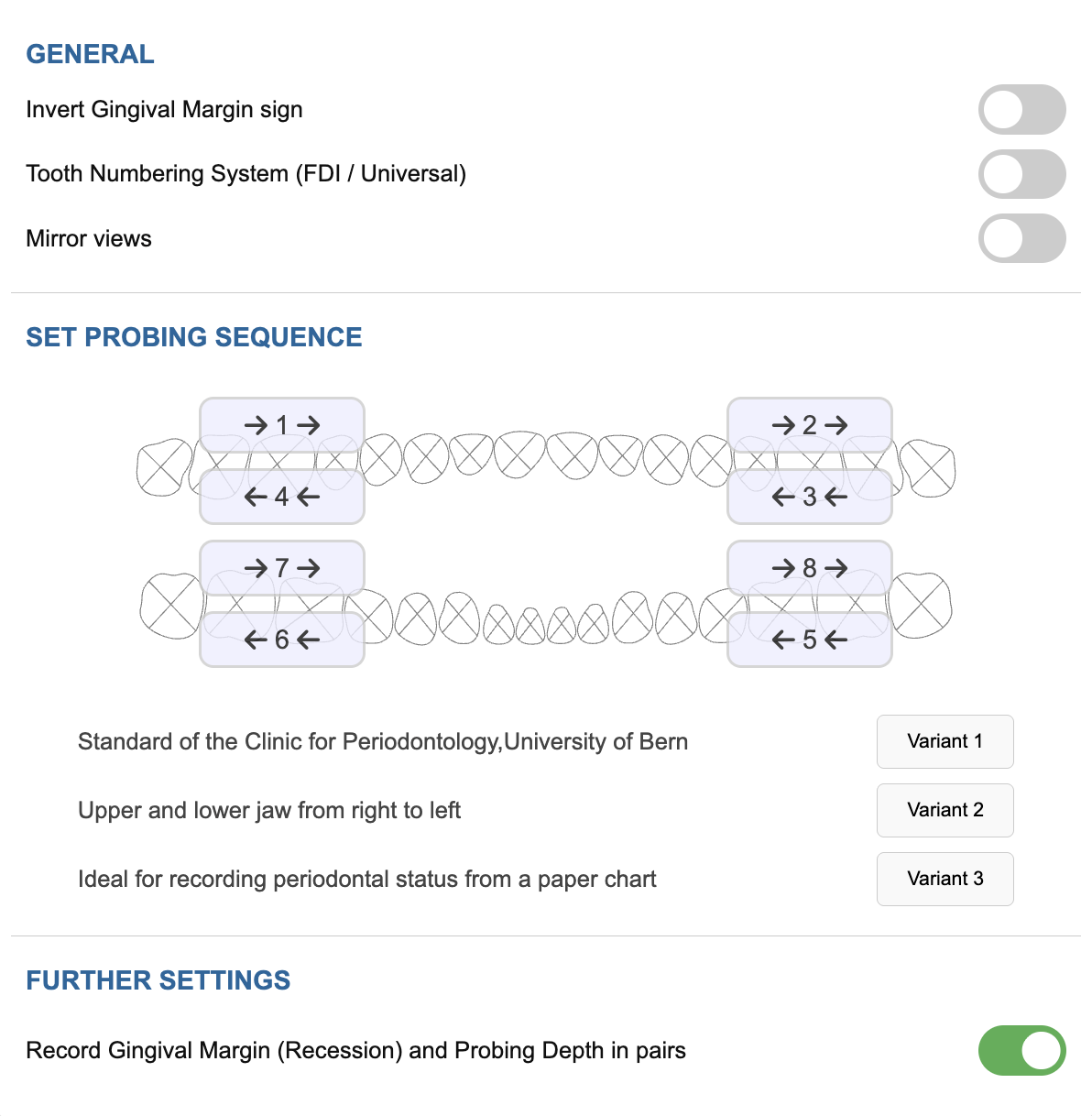
- Reverse Gingival Margin Signs: Toggle whether negative or positive values represent recession.
- Tooth Numbering System: A toggle slider button allows switching between the FDI and the Universal tooth numbering system.
- Mirroring Tooth Orientation: Maxillary teeth display roots upward, mandibular teeth downward.
- Probing Sequence: Arrows representing the probing direction can be customized via drag and drop, globally or per chart.
- Pairwise Data Entry: Facilitates entering GM and PD consecutively for each site.
Controls
Multiple controls highlight specific clinical parameters or handle image exports:
- Image Export: Download the current view (Full, Maxilla, or Mandible) as an image.
- Plaque and Bleeding Visualizations: Quickly highlight sites according to established index systems.
- Deep Probing Sites: Highlight depths ≥5 mm and ≥6 mm to identify residual pockets.
Periodontal Risk Assessment (PRA)
This button opens www.perio-tools.com with the parameter i and the values from the present exam.
https://www.perio-tools.com/pra/?lang=en&i=0000000032000Periodontal Classification
Provides an automatic diagnostic suggestion (Stage and Grade) according to Tonetti et al. (2018). The system analyzes clinical parameters such as molar-incisor patterns, probing depth distribution, smoking status, and diabetes stability.
Overview
A visualization focusing on Plaque Index (PI%) and Bleeding on Probing (BOP%) for the current record. The overview can be downloaded as an image.
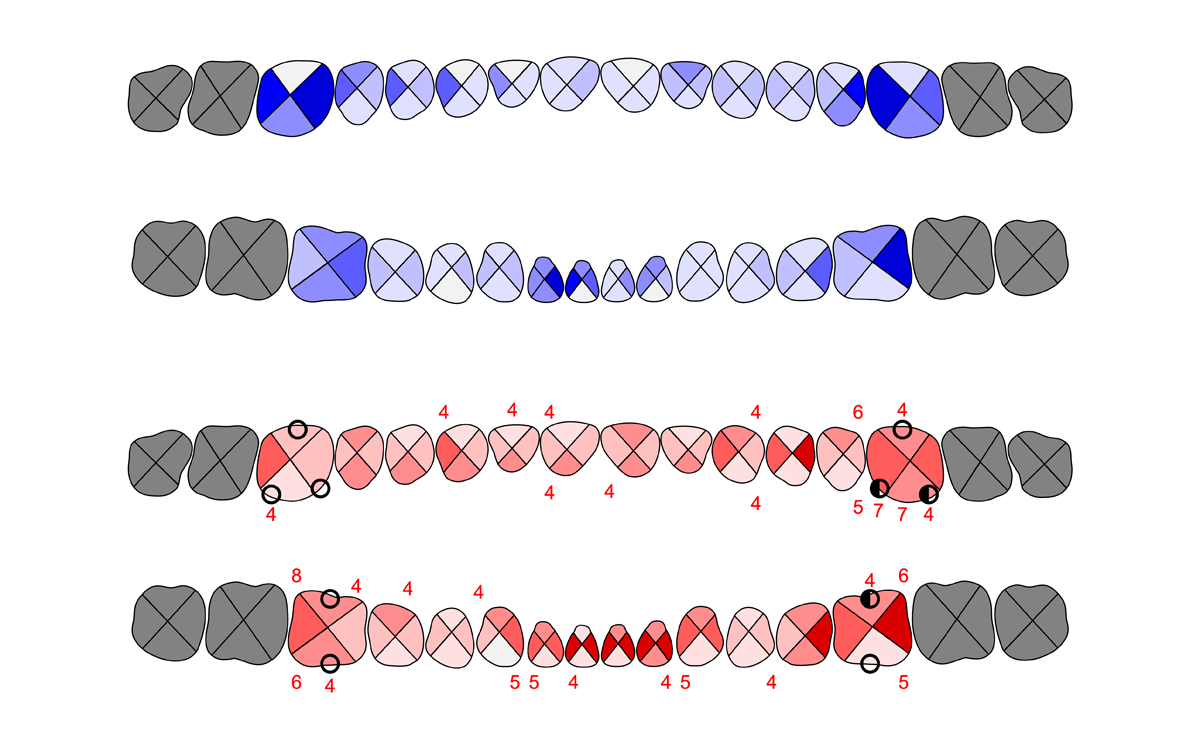
Analysis (Comparative View)
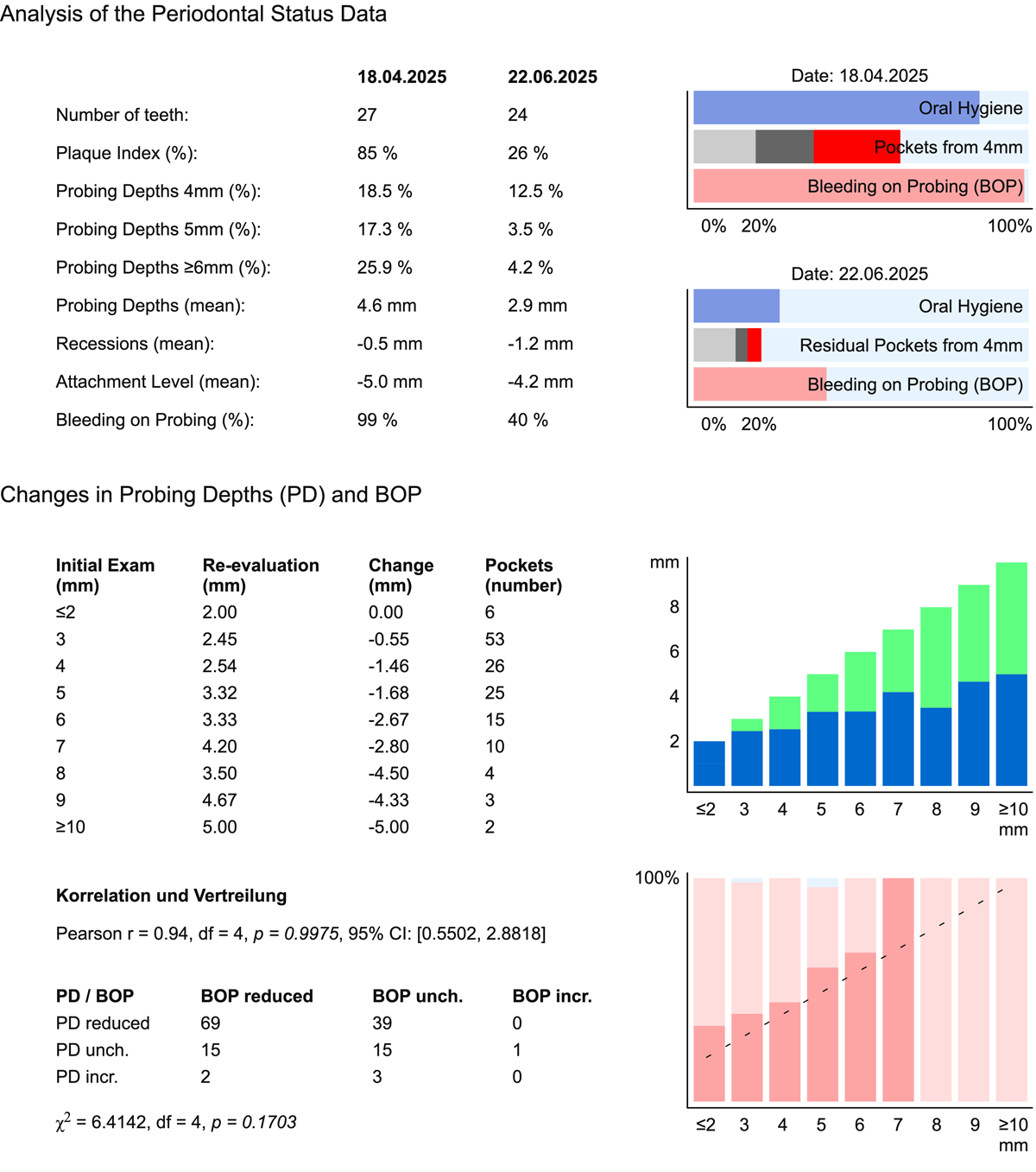
The system provides a comprehensive comparison between both examinations:
- Color Coding: Green indicates clinical improvement, blue represents residual probing depths, and red highlights clinical worsening.
- Bleeding Change: A dashed diagonal line represents the expected correlation between probing depth and bleeding. The analysis tracks the shift in bleeding intensity, statistically confirmed by a Chi-square test.
Recall Interval
Determines the recommended recall schedule based on Ramseier et al. (2019). The risk calculation includes the probing profile, systemic factors (Smoking, Diabetes), and Furcation involvement (Degree ≥2). Results are downloadable as an image.
3D Visualization
Renders a 3D model of the periodontal surface area, documenting the Total Periodontal Surface Area (TPSA) in cm² and analyzes BOP-positive vs. BOP-negative surfaces. The model can be zoomed, rotated, and exported as a GLTF file for Virtual Reality (VR) or Augmented Reality (AR) applications.
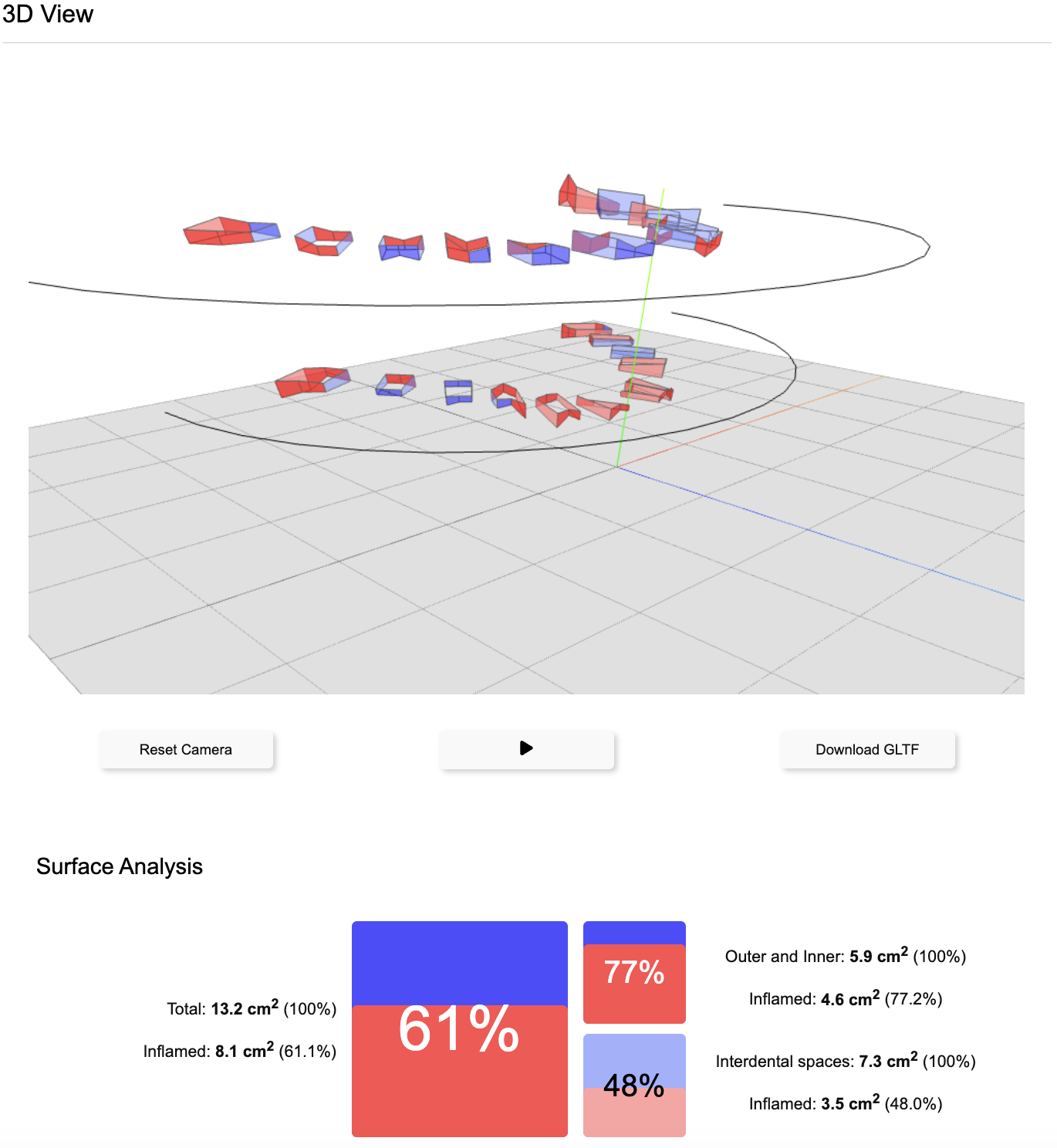
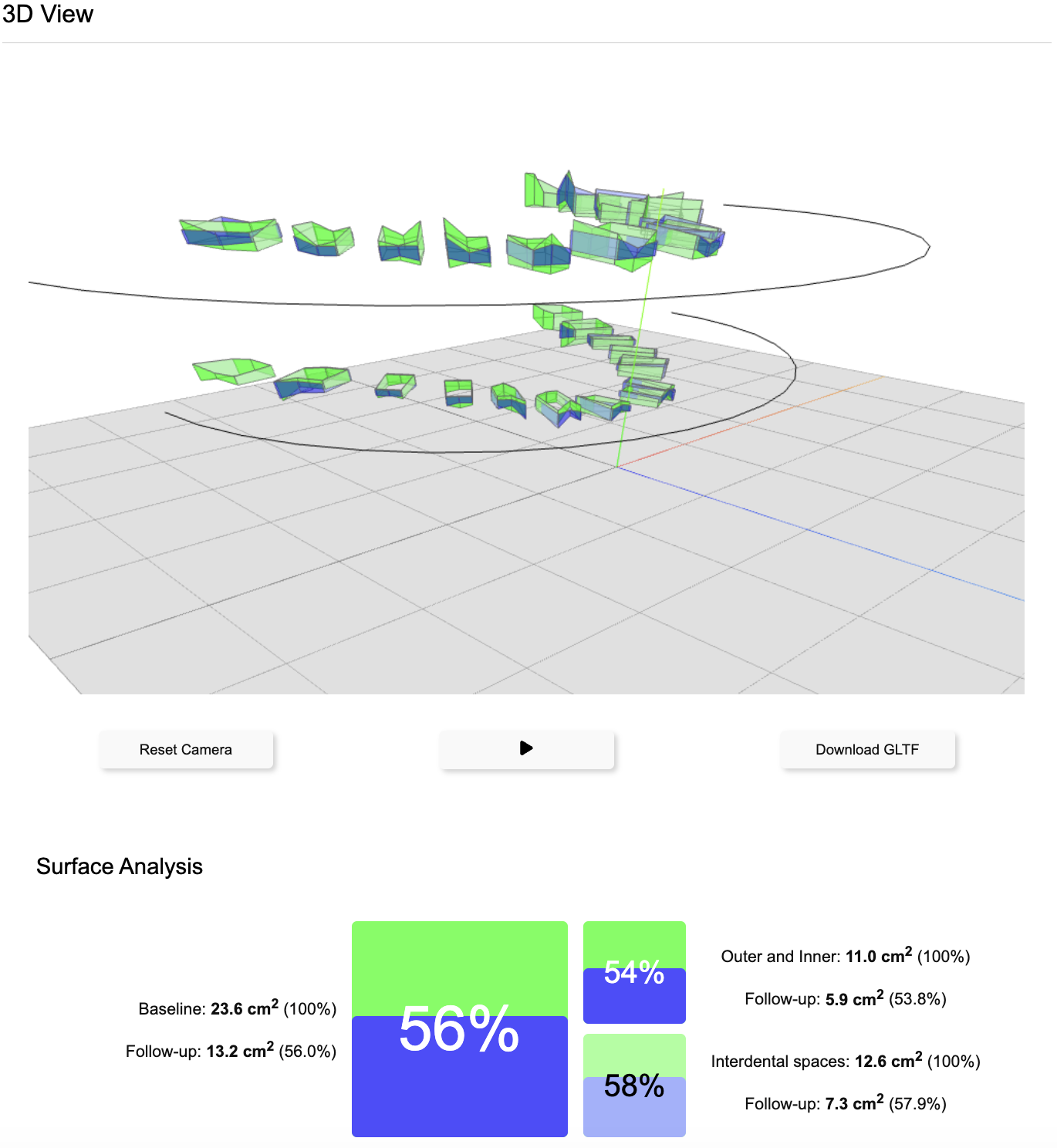
QR Code Sharing
Generates a QR code for the current chart, allowing it to be shared and viewed on mobile devices via a responsive web viewer on mobile devices.
Examiner Calibration
Used to evaluate consistency between two measurements (intra- or inter-examiner). The system calculates the Intra-class Correlation Coefficient (ICC) and provides Bland-Altman plots. This is particularly valuable for ensuring measurement reliability in clinical studies.
API Access
The aim of this API is to make the online Periodontal Chart accessible from external applications (e.g., dental practice software). Via a generated link, anonymized findings data are transferred and visualized directly in the viewer.
Base URL
https://www.periodontalchart-online.com/api/Query String Parameters
The query string is transmitted via the i parameter. This contains the anonymized and compressed data of the online Periodontal Chart.
Example URL
https://www.periodontalchart-online.com/api/?i=5051505050...Detailed technical documentation of the API can be found here: API Documentation.
3. General Health Tab
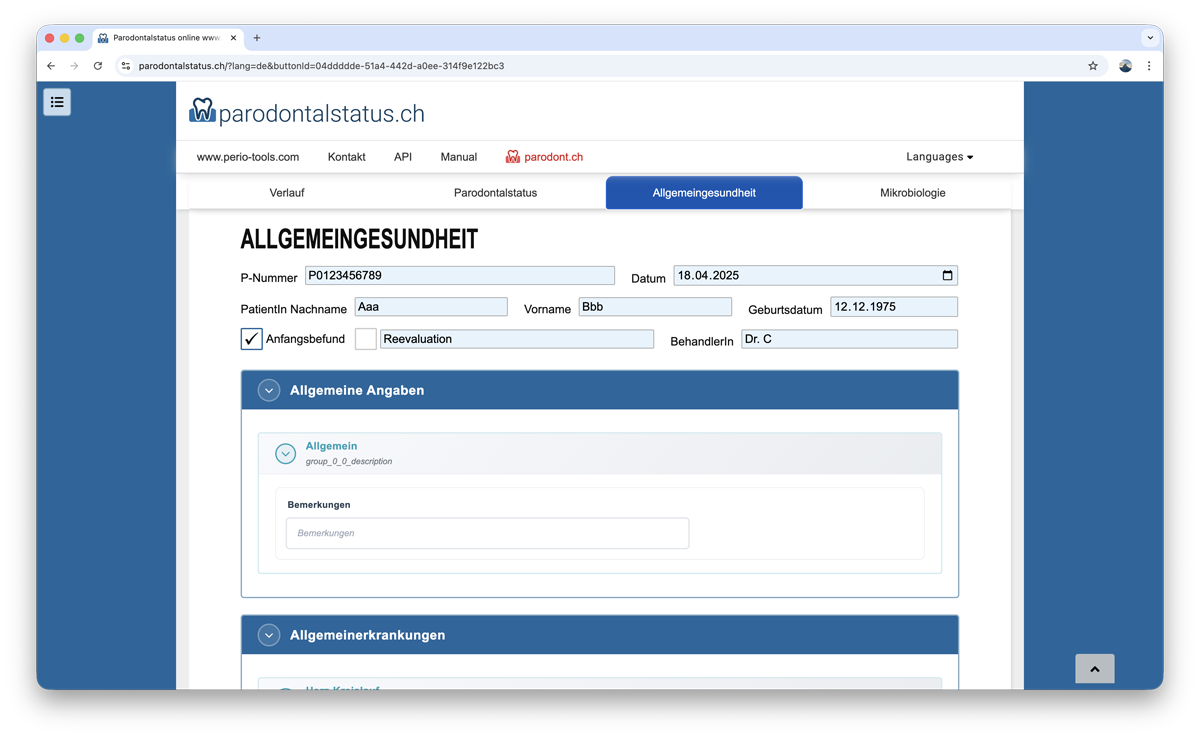
Questionnaire Structure
The list includes a wide range of medical questions that can be expanded or collapsed as needed. Individual health areas are organized into sections that can be managed independently for better overview.
Data Persistence and Export
For each chart, all selections in the health questionnaire are individually saved and timestamped. This data is fully integrated into the Data Export function, allowing medical information to be analyzed statistically alongside clinical periodontal parameters.
Customization (Questionnaire Editor)
The entire questionnaire can be fully customized using the Editor button:
- Editing: Add new questions, create custom dropdown menus, or define new categories.
- Flexibility: Entirely new health forms can be created, making the application ideal for collecting specific data in clinical studies.
- Reset: If needed, the questionnaire can be restored to its default state at any time.
4. Microbiology Tab
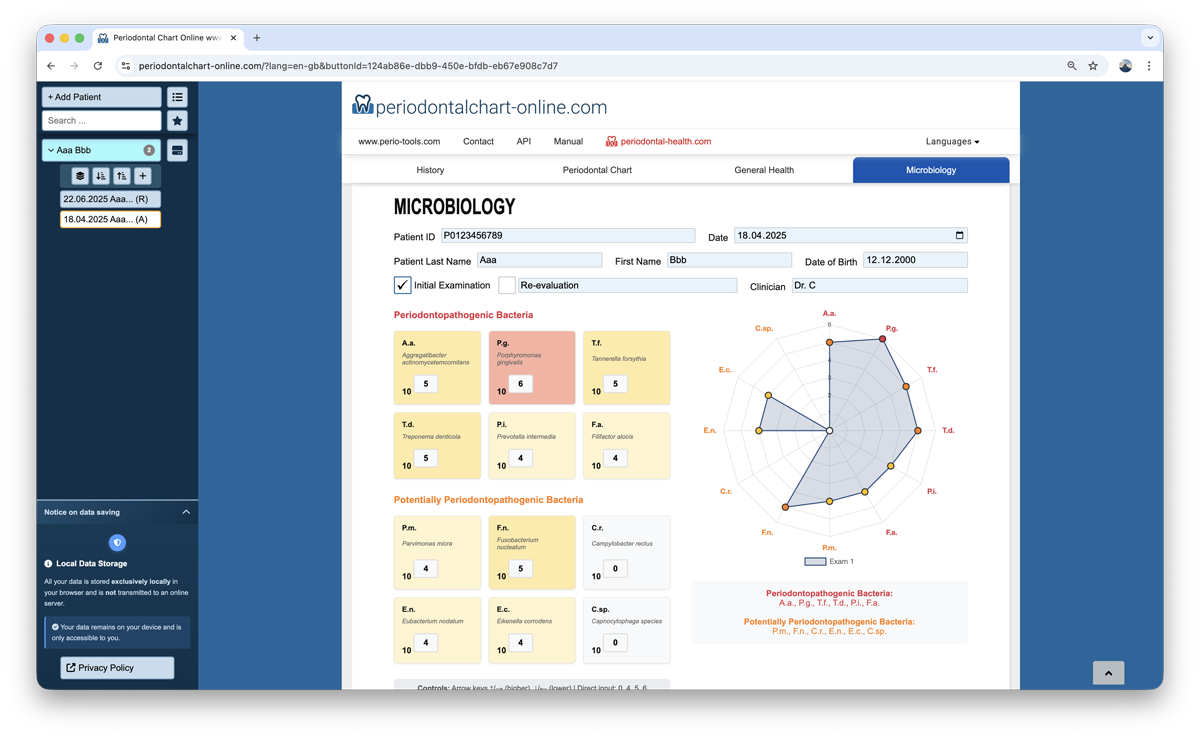
Pathogen Recording
The system allows recording load levels for 12 different pathogens. Data entry is based on exponents (e.g., entering 4, 5, or 6 to represent 104, 105, or 106). A value of 0 indicates the pathogen was not detected.
Visualization (Polygon Diagram)
The findings are visualized in a 12-sided polygon diagram (spider chart), providing an immediate overview of the microbiological profile of the patient.
Microbiological Shift (Comparative View)
When two charts are selected for comparison (using SHIFT+Click in the navigation panel), the microbiology tab visualizes the shift between the two time points:
- Green Shading: Represents the microbiological profile of the first examination.
- Blue Shading: Represents the profile of the second (follow-up) examination.
This overlay makes it easy to visualize the reduction or clinical shift of pathogens following treatment.
5. History Tab
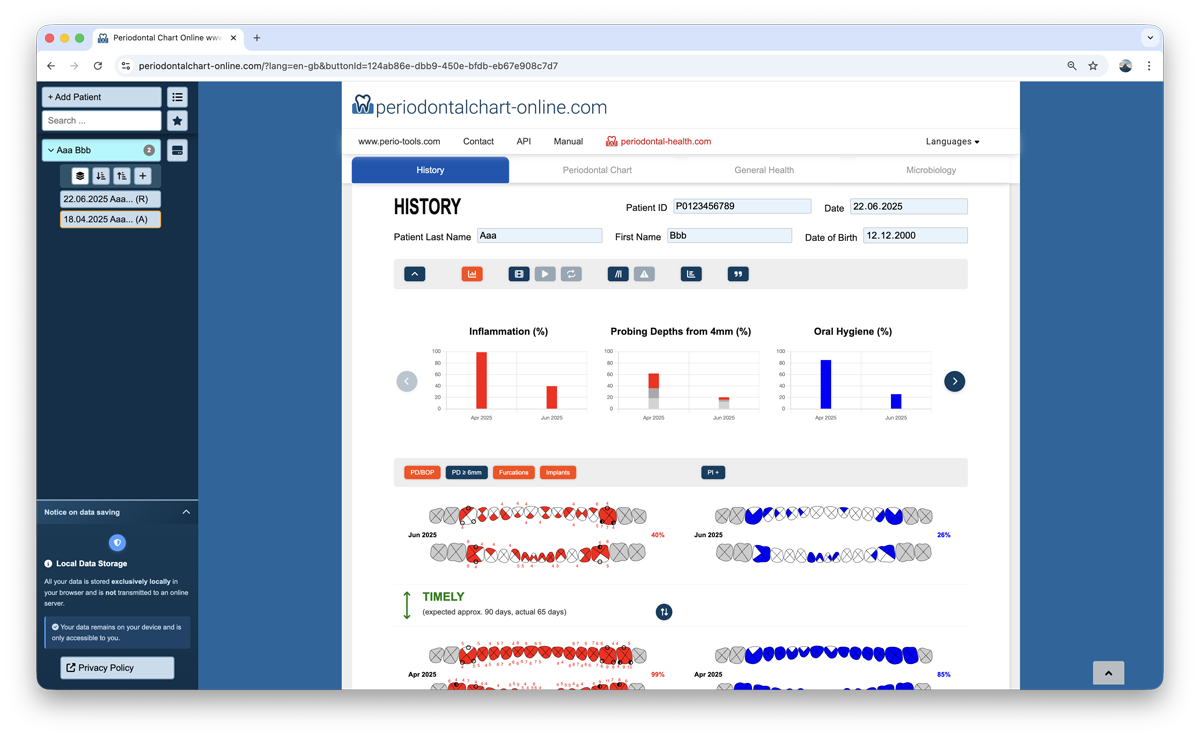
The History tab provides a comprehensive longitudinal view of all periodontal examinations for a patient, displayed in reverse chronological order (latest chart first).
Comparative Visualization
Each record displays the Probing and Bleeding findings on the left and the Oral Hygiene (Plaque) findings on the right, side by side for easy comparison.
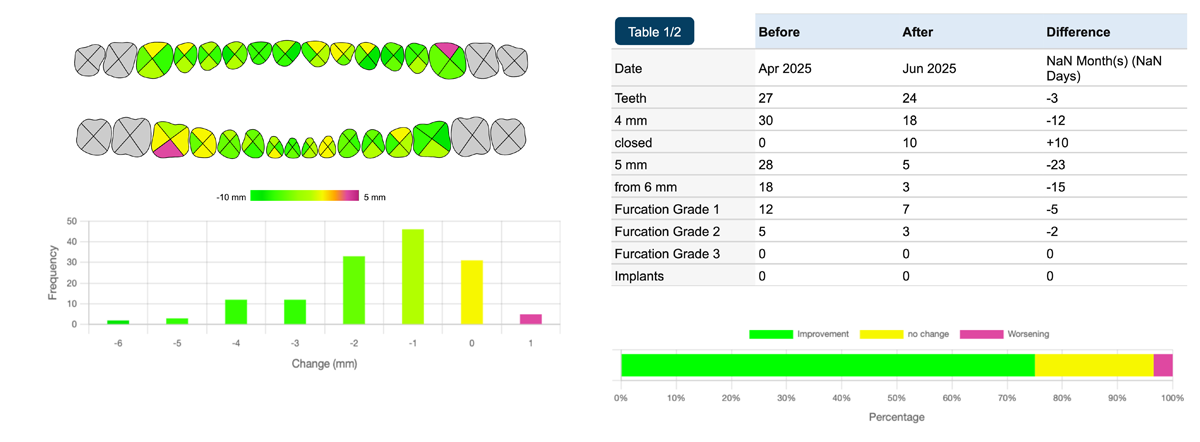
Change Analysis (Arrow Buttons)
Clicking the arrow buttons between two charts inserts a visual analysis of clinical changes:
- Color Coding:
- Green/Light Green: Significant clinical improvement.
- Yellow: Stable (no change).
- Pink/Dark Pink: Clinical worsening in probing depths.
- Closed Pockets: The analysis identifies "Closed Pockets," defined as sites with a probing depth of ≤4 mm and no bleeding on probing (BOP).
- Ranking Tables: Use the toggle to switch between distribution data (Table 1) and a ranking of sites with the greatest treatment need (Table 2).
Interactive Tools
- Animation Loop: Use the Play/Pause/Loop buttons to visualize the progression of periodontal disease and healing through a time-lapse overlay.
- Heatmap: Highlights sites with frequent bleeding or plaque across multiple examinations.
- Risk Indicators: The exclamation mark button highlights sites with repeated bleeding (BOP), indicating an increased risk for further attachment loss (Lang 1986).
Reports and AI Integration
- Stability Evaluation: Generates a patient-friendly report in accessible language regarding the current periodontal stability and recommended recall profile.
- AI Clinical Report: The AI Button generates an anonymized clinical prompt based on the patient's findings. Users can copy this prompt or open Google Gemini directly to generate a natural-language clinical report via copy-paste.
6. Literature
The following scientific references were used to establish the clinical indices and algorithms within the online periodontal chart tool:
- Textbook of Periodontia. 3rd ed. Miller SC (1950). Philadelphia: Blakiston.
- Löe H, Silness J. Periodontal Disease in Pregnancy. I. Prevalence and Severity. Acta Odontol Scand. 1963;21:533-551
- Silness J, Löe H. Periodontal Disease In Pregnancy. Ii. Correlation Between Oral Hygiene And Periodontal Condtion. Acta Odontol Scand. 1964;22:121-135
- O'Leary TJ, Drake RB, Naylor JE. The plaque control record. J Periodontol. 1972;43:38
- Miller PD, Jr. A classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985;5:8-13
- Lang NP, Joss A, Orsanic T, Gusberti FA, Siegrist BE. Bleeding on probing. A predictor for the progression of periodontal disease? J Clin Periodontol. 1986;13:590-596
- Mombelli A, van Oosten MA, Schurch E, Jr., Land NP. The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol Immunol. 1987;2:145-151
- Cairo F, Nieri M, Cincinelli S, Mervelt J, Pagliaro U. The interproximal clinical attachment level to classify gingival recessions and predict root coverage outcomes: an explorative and reliability study. J Clin Periodontol. 2011;38:661-666
- Pandey S, Mehta DS. Treatment of localized gingival recession using the free rotated papilla autograft combined with coronally advanced flap by conventional (macrosurgery) and surgery under magnification (microsurgical) technique: A comparative clinical study. J Indian Soc Periodontol. 2013;17:765-770
- Woelfel's Dental Anatomy. Schneid RC, Weiss G (2017). Philadelphia: Wolters Kluwer.
- Tonetti MS, Greenwell H, Kornman KS. Staging and grading of periodontitis: Framework and proposal of a new classification and case definition. J Periodontol. 2018;89 Suppl 1:S159-S172
- Ramseier CA, Nydegger M, Walter C, Fischer G, Sculean A, Lang NP, Salvi GE. Time between recall visits and residual probing depths predict long-term stability in patients enrolled in supportive periodontal therapy. J Clin Periodontol. 2019;46:218-230